

Severe obesity is a chronic condition that is very difficult to treat. Surgery to promote weight loss by restricting food intake or interrupting digestive processes is an option for severely obese people. A body mass index (BMI) above 40--which means about 100 pounds of overweight for men and about 80 pounds for women--indicates that a person is severely obese and therefore a candidate for surgery (see table 1). Surgery also may be an option for people with a BMI between 35 and 40 who suffer from life-threatening cardiopulmonary problems (for example, severe sleep apnea or obesity-related heart disease) or diabetes. However, as in other treatments for obesity, successful results depend mainly on motivation and behavior.

Normally, as food moves along the digestive tract (see figure 1), appropriate
digestive juices and enzymes arrive at the right place at the right time
to digest and absorb calories and nutrients. After we chew and swallow
our food, it moves down the esophagus to the stomach, where a strong acid
continues the digestive process. The stomach can hold about 3 pints of
food at one time. When the stomach contents move to the duodenum, the first
segment of the small intestine, bile and pancreatic juice speed up digestion.
Most of the iron and calcium in the foods we eat is absorbed in the duodenum.
The jejunum and ileum, the remaining two segments of the nearly 20 feet
of small intestine, complete the absorption of almost all calories and
nutrients. The food particles that cannot be digested in the small intestine
are stored in the large intestine until eliminated.
The concept of gastric surgery to control obesity grew out of results
of operations for cancer or severe ulcers that removed large portions of
the stomach or small intestine.
Because patients undergoing these procedures tended to lose weight after
surgery, some physicians began to use such operations to treat severe obesity.
The first operation that was widely used for severe obesity was the intestinal
bypass. This operation, first used 40 years ago, produces weight loss by
causing malabsorption. The idea was that patients could eat large amounts
of food, which would be poorly digested or passed along too fast for the
body to absorb many calories. The problem with this surgery was that it
caused a loss of essential nutrients and its side effects were unpredictable
and sometimes fatal. The original form of the intestinal bypass operation
is no longer used.
Surgeons now use techniques that produce weight loss primarily by limiting how much the stomach can hold. These restrictive procedures are often combined with modified gastric bypass procedures that somewhat limit calorie and nutrient absorption and may lead to altered food choices.
Two ways that surgical procedures promote weight loss are:
Although results of operations using these procedures are more predictable
and manageable, side effects persist for some patients.
Restriction Operations
Restriction operations are the surgeries most often used for producing
weight loss. Food intake is restricted by creating a small pouch at the
top of the stomach where the food enters from the esophagus. The pouch
initially holds about 1 ounce of food and expands to 2-3 ounces with time.
The pouch's lower outlet usually has a diameter of about 1/4 inch. The
small outlet delays the emptying of food from the pouch and causes a feeling
of fullness.
After an operation, the person usually can eat only a half to a whole cup of food without discomfort or nausea. Also, food has to be well chewed. For most people, the ability to eat a large amount of food at one time is lost, but some patients do return to eating modest amounts of food without feeling hungry.
Restriction operations for obesity include gastric banding and vertical banded gastroplasty. Both operations serve only to restrict food intake. They do not interfere with the normal digestive process.

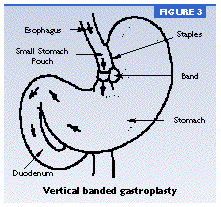
Restrictive operations lead to weight loss in almost all patients. However, weight regain does occur in some patients. About 30 percent of persons undergoing vertical banded gastroplasty achieve normal weight, and about 80 percent achieve some degree of weight loss. However, some patients are unable to adjust their eating habits and fail to lose the desired weight. In all weight-loss operations, successful results depend on your motivation and behaviors.
A common risk of restrictive operations is vomiting caused by the small stomach being overly stretched by food particles that have not been chewed well. Other risks of VBG include erosion of the band, breakdown of the staple line, and, in a small number of cases, leakage of stomach juices into the abdomen. The latter requires an emergency operation. In a very small number of cases (less than 1 percent) infection or death from complications can occur.
Gastric Bypass Operations
These operations combine creation of small stomach pouches to restrict
food intake and construction of bypasses of the duodenum and other segments
of the small intestine to cause malabsorption.

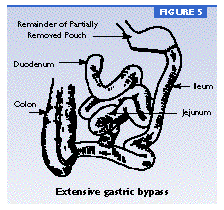
Gastric bypass operations (figures 4 and 5) that cause malabsorption and restrict food intake produce more weight loss than restriction operations (figures 2 and 3) that only decrease food intake. Patients who have bypass operations generally lose two-thirds of their excess weight within 2 years.
The risks for pouch stretching, band erosion, breakdown of staple lines, and leakage of stomach contents into the abdomen are about the same for gastric bypass as for vertical banded gastroplasty. However, because gastric bypass operations cause food to skip the duodenum, where most iron and calcium are absorbed, risks for nutritional deficiencies are higher in these procedures. Anemia may result from malabsorption of vitamin B12 and iron in menstruating women, and decreased absorption of calcium may bring on osteoporosis and metabolic bone disease. Patients are required to take nutritional supplements that usually prevent these deficiencies.
Gastric bypass operations also may cause "dumping syndrome," whereby stomach contents move too rapidly through the small intestine. Symptoms include nausea, weakness, sweating, faintness, and, occasionally, diarrhea after eating, as well as the inability to eat sweets without becoming so weak and sweaty that the patient must lie down until the symptoms pass.
The more extensive the bypass operation, the greater is the risk for
complications and nutritional deficiencies. Patients with extensive bypasses
of the normal digestive process require not only close monitoring, but
also life-long use of special foods and medications.
Surgery to produce weight loss is a serious undertaking. Each individual should clearly understand what the proposed operation involves. Patients and physicians should carefully consider the following benefits and risks:
Benefits
Risks
For patients who remain severely obese after nonsurgical approaches to weight loss have failed, or for patients who have an obesity-related disease, surgery may be the best next step. But for other patients, greater efforts toward weight control, such as changes in eating habits, behavior modification, and increasing physical activity, may be more appropriate. Answers to the following questions may help in your decision to undergo surgery for weight loss.
Are you:
Do you:
Remember: There are no guarantees for any method, including surgery,
to produce and maintain weight loss. Success is possible only with your
fullest cooperation and commitment to behavioral change and medical followup--and
this cooperation and commitment should be carried out for the rest of your
life.
NIH Publication No. 96-4006
April 1996
The content on NetMedicine is intended solely for informational purposes and is in no way intended to be used for making decisions about your healthcare. There is no substitute for discussing your medical and health-related needs with your physician.
Design is copyright © 1996 Triple Star Systems, Inc.