The ECG is a medical device capable of recording the
electrical activitity of the heart from
electrodes placed on the skin in specific locations.
Some of the first EKG machines were bulky,
table-sized apparatus built about 1920.
Early EKG Machine

Today's units are compact, lightweight and placed on
carts which can be wheeled to any location in
the hospital. One of the biggest and best improvements on these early machines
came with the invention of the electrode, the p[art that conducts the heart's
electrical activity to the machine. In the early
1900s, hands and feet were placed in sodium chloride baths
as a means of conduction, but by the
1940s metal disks with wire leads were strapped to wrists
and ankles. Now, the wire leads are
attached to disposable patches which are
self-adhesive.
Patient demonstrating early EKG machine

Pics courtesy of the University of Iowa Hospital and Medical Clinics



The electrocardiogram is still the basic cardiologic
test and is widely
applied in patients with suspected or known heart disease
and as a basic
reference for most other cardiologic tests.
USES:
 In patients without known heart disease, the ECG is used
as a screening test
for coronary artery disease, cardiomyopathies, or
left ventricular
hypertrophy and is then used as a baseline for future
reference and comparison.
In patients without known heart disease, the ECG is used
as a screening test
for coronary artery disease, cardiomyopathies, or
left ventricular
hypertrophy and is then used as a baseline for future
reference and comparison.
 Preoperatively, it is used to rule out silent coronary artery
disease. This is very important as the presence of disease can cause complications with
arrythmias during surgery and after, as well as anesthesia problems. It will not,
definately rule out the surgery, if disease is present, but will help staff to be better prepared for what
may happen. If it is bad enough, however, it can be a deciding factor.
Preoperatively, it is used to rule out silent coronary artery
disease. This is very important as the presence of disease can cause complications with
arrythmias during surgery and after, as well as anesthesia problems. It will not,
definately rule out the surgery, if disease is present, but will help staff to be better prepared for what
may happen. If it is bad enough, however, it can be a deciding factor.
 The ECG may
also provide information in the presence of metabolic
alterations, such as
hypercalcemia and hypocalcemia and hyperkalemia and
hypokalemia.
The ECG may
also provide information in the presence of metabolic
alterations, such as
hypercalcemia and hypocalcemia and hyperkalemia and
hypokalemia.
 In
patients with known heart disease, the ECG serves as a
baseline for the
severity and progression of the disease process. The ECG
is invaluable in the
evaluation of patients with chest pain and in the
management of patients with
suspected or known to have acute myocardial infarction
or coronary
insufficiency. Most patients with myocardial, valvular,
and congenital heart
disease will eventually demonstrate ECG abnormalities.
In
patients with known heart disease, the ECG serves as a
baseline for the
severity and progression of the disease process. The ECG
is invaluable in the
evaluation of patients with chest pain and in the
management of patients with
suspected or known to have acute myocardial infarction
or coronary
insufficiency. Most patients with myocardial, valvular,
and congenital heart
disease will eventually demonstrate ECG abnormalities.
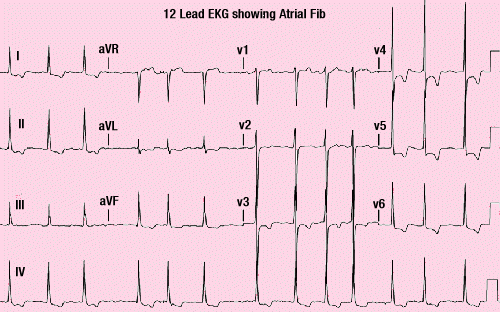
 Rhythm disorders can effectively be evaluated through an
ECG rhythm strip. This can be done with bedside EKG monitoring
or "telemetry", but is much better seen and diagnosed with a 12 lead EKG,
as many views of the heat can be viewed all at once.
Rhythm disorders can effectively be evaluated through an
ECG rhythm strip. This can be done with bedside EKG monitoring
or "telemetry", but is much better seen and diagnosed with a 12 lead EKG,
as many views of the heat can be viewed all at once.

CONTRAINDICATIONS
 There are no contraindications for ECG recordings. Everyone gets to benefit from this
wonderful test!
There are no contraindications for ECG recordings. Everyone gets to benefit from this
wonderful test!
|
|
|
|
|
|
|
|
|
|
 There are no contraindications for ECG recordings. Everyone gets to benefit from this
wonderful test!
There are no contraindications for ECG recordings. Everyone gets to benefit from this
wonderful test!
PATIENT PREPARATION
 There is no special patient preparation is needed, patients do not
need to fast before
the ECG is taken and no special time of the day is
preferable.
There is no special patient preparation is needed, patients do not
need to fast before
the ECG is taken and no special time of the day is
preferable.
SETTING UP THE EKG
 Inpatients
will have a bedside ECG and outpatients will
go to the ECG
Laboratory. Patients can be scheduled to have a routine
ECG or stat ECG to be done
immediately. The reason
for the request should be noted in the chart or in the
requisition form.
Additional information of interest includes patient's
age, sex, and race, as well
as any cardiac medications they may be taking.
Inpatients
will have a bedside ECG and outpatients will
go to the ECG
Laboratory. Patients can be scheduled to have a routine
ECG or stat ECG to be done
immediately. The reason
for the request should be noted in the chart or in the
requisition form.
Additional information of interest includes patient's
age, sex, and race, as well
as any cardiac medications they may be taking.
 Situations
that require special
lead placement should be noted. These include use of back
leads if a posterior
myocardial infarction is suspected and use of right
precordial leads if a right
ventricular infarction is suspected. If the patient has
a rhythm disturbance a
rhythm strip may be requested.
Situations
that require special
lead placement should be noted. These include use of back
leads if a posterior
myocardial infarction is suspected and use of right
precordial leads if a right
ventricular infarction is suspected. If the patient has
a rhythm disturbance a
rhythm strip may be requested.
 After
checking the appropriateness and type of ECG to be
taken, let your pateint know what you are doing. When he/she
understands
and is agreeable to the procedure, you may begin your lead
placement.
After
checking the appropriateness and type of ECG to be
taken, let your pateint know what you are doing. When he/she
understands
and is agreeable to the procedure, you may begin your lead
placement.
 With the patient in a
supine and relaxed position, the wrists and ankles are
prepared for the
extremity leads.
With the patient in a
supine and relaxed position, the wrists and ankles are
prepared for the
extremity leads.

The precordium is prepared for
the precordial
leads and the electrodes are put in place with contact gel.
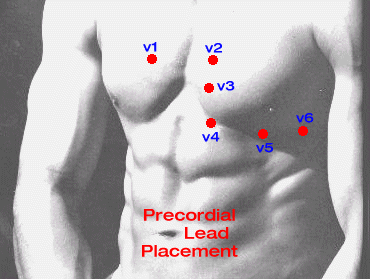
If a machine with
non-disposible suction cups is used, then the leads are
supported by
elastic straps in the extremities.
 Occasionally, areas of the limbs and chest need to be
shaved to provide good contact. Use your judgement here..but remember, the more hair,
the more interference....
Occasionally, areas of the limbs and chest need to be
shaved to provide good contact. Use your judgement here..but remember, the more hair,
the more interference....
 After
making sure that your leads are attached properly, and that
the calibration settings are adequate,
you may begin recording your EKG. This can be done by selecting
lead by
lead (on older machines) or, with the
newer ECG recorders, by simultaneous recordings of 3-6
leads. The
recordings are usually made at a paper speed of
25 mm/second. Usually one
copy is left in the chart and/or is given to the patient and
one copy goes to the
ECG Laboratory for interpretation and findings.
After
making sure that your leads are attached properly, and that
the calibration settings are adequate,
you may begin recording your EKG. This can be done by selecting
lead by
lead (on older machines) or, with the
newer ECG recorders, by simultaneous recordings of 3-6
leads. The
recordings are usually made at a paper speed of
25 mm/second. Usually one
copy is left in the chart and/or is given to the patient and
one copy goes to the
ECG Laboratory for interpretation and findings.

The precordium is prepared for the precordial leads and the electrodes are put in place with contact gel.

If a machine with non-disposible suction cups is used, then the leads are supported by elastic straps in the extremities.



First, let's review the Conduction Systems of the Heart:
| First wave of complex |
1.Is negative/below isoelectric line 2.Must be first wave of complex and must be negative and small 3.Amplitude (normal q wave) is less than one fourth height of its R-wave |
|
| R wave |
1.Is always positive (above isoelectric line) 2.No such thing as a "negative R-wave" |
|
| S wave | 1. Is a negative deflection following the R wave. | |
| T wave |
1. Represents ventricular repolarization 2. Normal T waves are in the same direction as their complex 3. Normal T wave is asymmetrical and it peaks toward the end, instead of the middle. 4. Normal T: in frontal plan <= 5mm, in precordial plane <= 10mm tall. |
|
| ST Segment |
1. Is measured from the end of complex to the beginning of T wave 2. ST is the beginning of ventricular repolarization 3. Normal ST is on the isoelectric line or no more than 1mm above or below isoelectric line 4. Elevated ST is more than 1mm above isoelectric line 5. Depressed ST is more than 1 mm below isoelectric line |
|
| PRI (normal PRI 0.12 - .20 seconds) |
1. Normal PRI is measured from beginning of the P to the beginning of
the complex 2. This measurement represents the time it takes for a wave of depolarization to spread through the atria, AV node, and AV junction |
Paper and Voltage
Each small box on the horizontal line represents 0.04 seconds. Each large box on the horizontal line represents 0.20 seconds. There are five small boxes in one large box. Each small box on the vertical line equals 0.1 millivolts. 10 small boxes = 10 mm tall.
Leads, Lead Placement, Precordial Leads
The activity of the heart produces electrical potentials, which can be measured on the surface of the body.
or "What Kind Of MI Is This???
| Inferior Leads |
1.RCA supplies the inferior wall of the ventricle 2.MI's involving inferior surface of the heart will be seen in leads II, III, and aVF |
| Lateral Leads |
1.Leads I, aVL, V5, V6. 2.Lateral infarctions are usually associated with obstruction of the left circumflex artery. |
| Septum and Anterior Leads |
1.Intraventricular septum - leads V1 and V2. 2.Anterior Wall - V2, V3, V4. 3.Anterior infarctions are usually associated with occlusion of the left anterior descending branch of the left coronary artery. |
The three EKG changes are:
| Elevated ST segments (myocardial injury) |
1.Normal ST segments are in the isoelectric line or no more than 1mm
above or below it. 2.An abnormal electrical charge is produced on membrane of myocardial cell resulting in abnormal current flow causing an elevation of ST segment. 3.Myocardial injury causes elevation of ST segments over affected area of the ventricle. ST segments changes are the earliest indication on EKG. 4.ST segment changes occur within a few hours or a few days and should return to the isoelectric line within 2 weeks. |
| Inverted T waves (myocardial ischemia) |
1.Myocardial ischemia causes symmetrical inversion of the T wave. T wave abnormalities
reflect a change in ventricular repolarization. 2.As the ST segment begins to return to the isoelectric line, the symmetrical inversion of the T wave appears. 3.The T wave will become progressively deeper as the ST segment returns to the isoelectric line. |
| Pathological Q waves (myocardial infarction) |
1.Normal Q waves are small, less than 1 mm deep or wide and one fourth the height of
their R wave. 2.Pathological Q waves usually develop when ST segments are elevated and appear several hours or days after the clinical manifestations of the MI. 3.Abnormal Q must be one small square (0.04 sec) wide and greater than one-third of QRS height in Lead III. 4.Myocardial infarction causes pathological Q waves over the affected area of the ventricle. The age of the infarction can be determined. a.Q waves only - old infarction b.Q waves with elevated ST segments (with or without T wave inversion) - acute infarction c.Q waves with inverted T waves - age undetermined. |
Transmural MI- involves the full thickness of myocardium. EKG changes in transmural MI occur both in depolarization -q wave and repolarization -ST-T.
Nontransmural MI- does not involve the full thickness of myocardium. Also called subendocardial. Changes occur in ST-T wave.
| hyperacute phase | ST elevation and upright T waves. Occurs in first few hours and lasts 1-6 weeks. ST elevation beyond 6 weeks - suspect ventricular aneurysm. |
| fully evolved phase | after hours or days. Deep T waves and appearance of diagnostic q waves. |
| resolution phase | T waves return to normal within weeks to months. |
| stabilized chronic phase | q waves remain permanent |
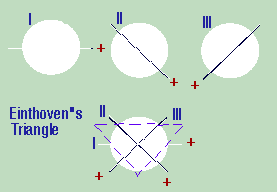
Determining the axis is dependent on understanding the angles that each of the chest leads make in relation to each other.
When trying to determine the axis, the leads that are important are the limb leads. The basic principle behind finding the axis is that you must look for the lead whose QRS complex is closest to zero or equiphasic (i.e., when the areas under each component of the QRS are added up (with those above baseline being positive and that below baseline negative, you get an approximate negative or positive value or zero).
This axis represents the lead that is perpendicular to the main axis of the ECG. Then to find the lead which is closest to the axis of the ECG, it is necessary to know how the leads are in relation to each other.
With this lead (i.e. the lead that was perpendicular to the lead which was equiphasic), you have a general idea of what the axis is. Each lead has a positive and negative pole, and therefore after you look at this lead on the ECG and determine whether the QRS complex is overall negative or positive, you need simply look at an axis diagram to determine what the axis is (corresponding with the positive or negative pole of that lead).
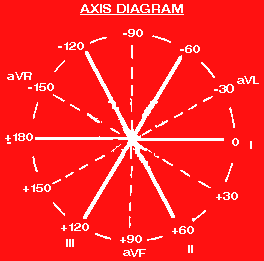
Since it will be unusual that any of the lead's QRS complex will equal zero, it is only necessary to know which is closest to zero. Since it isn't equiphasic, that means that this lead is not perfectly perpendicular to the axis of the ECG. This will be helpful in that after you do the other steps of finding which lead is perpendicular to the "equiphasic lead", you use the original equiphasic lead to "skew" the axis toward it by 10 degrees.
Morphology Determination By Axis
| P Wave Morphology |
The P wave in general should not be more than 1 box wide or 1 box tall.
If it exceeds these, it
generally means that either or both atria is enlarged (hypertrophied).
The best lead to look at the P wave is V1. In lead V1, the following
characteristics indicate
pathology: 1.Positive deflection greater than 1 box wide or 1 box in height --> right atrial hypertrophy 2.Total P wave duration greater than 0.12 sec and negative deflection of P wave greater than 1 box wide or 1 box in depth --> left atrial hypertophy |
| PR Interval |
The PR interval indicates AV conduction time which is normally between
0.12 - 0.20 msec (3 - 5
boxes wide). If the PR interval is greater than 0.2 sec, then an AV block
is present. There are
several types of AV blocks: 1st degree AV Block: PR>0.20 sec. 2nd degree AV Block: 2 types: a.Type I (Mobitz I or Wenckeback): increasing PR interval until a QRS complex is dropped. It is usually benign. b.Type 2 (Mobitz II): QRS dropped without any progressive increase in PR interval (i.e., PR interval is constant but still >0.20 sec). 3rd degree AV Block: atria and ventricles are electrically dissociated. Therefore, P waves and QRS complexes will occur independent of each other. As always, use the QRS complexes to determine heart rate. ***A PR interval that is <0.12 sec (when associated with a prolonged QRS) should prompt evaluation for Wolff-Parkinson-White Syndrome (WPW).*** |
| QRS Morphology |
The QRS complex can be quite difficult to interpret. However, stepwise
evaluation will make it
easier. The things to consider are the following: Duration: should be 0.08 - 0.10 sec (2 - 2.5 boxes). If duration is prolonged, then the presence of bundle branch blocks and WPW (if PR interval is also abnormally shortened in duration). Presence of Q waves: can indicate presence of infarct if present in V1, V2, and V3. A Q wave in III and aVR is normal. A Q wave is significant if it is greater than 1 box wide or greater than 1/3 the amplitude of the QRS complex. |
| ST Segment Morphology |
The ST segment is important because it can show whether ischemia or
infarct is present. In general,
an ST segment depression indicates ischemia while elevation generally
indicates infarction. When
examining the ST segment, evaluate elevations or depressions 0.06 seconds
after the J point (since
the ST segment can at times be sloping). The location of the ST elevations
on the ECG can help to
identify a location of the infarct: Anterior Wall Infarct (corresponding to Left Anterior Descending Artery): V1, V2 Lateral Wall Infarct (Circumflex Artery): V3, V4 Inferior Wall Infarct (can be combination of Circumflex or Right Coronary Artery): V5, V6, I, aVL ST depression in V1 and V2 associated with large R waves may indicate Posterior Wall infarction (corresponding with Right Coronary Artery). |
| T Wave Morphology |
In general, T waves are in the same direction as the largest deflection
of the QRS (normally the R
wave). The following pathology can be associated with T wave changes:
Ischemia: when T waves are in an opposite direction (inverted), it
may indicate that ischemia
is present, especially when it occurs in a pattern as previously
described for ST segment
changes. Hyperkalemia: associated with tall peaked T waves, flat P waves, and wide QRS complexes Hypokalemia:associated with flat T waves, U waves, U waves taller than T waves |
| U Wave Morphology | The presence of U waves may indicate hypokalemia. |
| QTc Interval |
May be lengthened in the following: Quinidine Toxicity Hypocalcemia May be shortened in hypocalcemia. |