Cardiac Auscultation
Of all the skills of the diagnostician
the auscultation of the heart is particular difficult to learn. I hope
that this page make it more easy to carry out.
Jos-paul Scholten.
The stethoscope
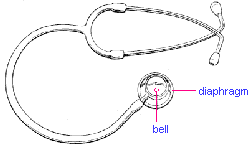
The bell, Is better for Low-pitched sounds, while
the high-pitched sounds are best heard with the diaphragm.
The technique
- Approach the patient from the right side.
- When using the bell, one must take care to exert
very little pressure.
- Excessive pressure converts the underlying skin
into a diaphragm and eliminates very low-pitched sounds.
- One must concentrate solely on each phase of
the cardiac cycle and each of the sounds separately.
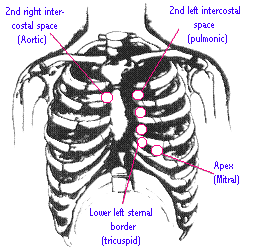
On auscultation one should first
try to discriminate :
- The heart sounds S1, S2 ,S3, S4
- Systolic sounds
- Diastolic sounds
- Continued sounds
At first listen to the S1 at every
location. Then listen to the S2. After they are recognised, listen to the
sounds witch are around the S1 and S2.
The 1st heart sound (S1)

It represents the closure of mitral
and tricuspid valves. It is best heard in mitral and tricuspid areas.
- Normal: Splitting in inspiration may be heart,
it has a high pitch.
- Loud: Mitral stenosis, tachycardia.
- Soft: Mitral regurgitation.
 Normal,
Normal,
 Splitted
S1,
Splitted
S1,  Wide
splitted S1.
Wide
splitted S1.
The 2nd heart sound (S2)

Represents the closure of the aortic
and pulmonary valves. It is best heard in the aorta and pulmonary areas.
- Normal : First aorta closure then pulmonary closure.
Delayed pulmonary closure in inspiration. (increased right ventricular
volume while decreased left ).
- Abnormally wide splitting: Late aorta closure
in left bundle branch block and aorta stenosis.
- Early pulmonary closure in pre-excitation phenomena.
- Late pulmonary closure in increased volume flow
through the right ventricle, such as atrial septum defect which is not
varying with respiration.
- Reverse splitting (splitting increasing on expiration
) : Left bundle branch block , systemic hypertension, aorta stenosis.
- Loud : Aorta closure, because of the systemic
hypertension and in pulmonary closure ( pulmonary hypertension ).
- Soft : Aorta closure, because of the aorta stenosis
and pulmonary closure ( pulmonary stenosis ).
 Splitted
S2,
Splitted
S2,  Wide
splitted 2S,
Wide
splitted 2S,  Reversed
splitting.
Reversed
splitting.
The 3rd heart sound (S3)

Occurs shortly after S2. It is early
diastolic and occurs during passive diastolic filling. It Is low pitched,
has a long duration and is best heard with the bell in the mitral and tricuspid
areas.
- S3 (Right ventricular) increase with inspiration.
- S3 (Left ventricular) increase with expiration.
- Normal : young people < 35 years.
- Abnormal : Left and right heart failure, mitral
regurgitation, constrictive pericarditis ( high pitched = is the pericardial
knock ).
 S3.
S3.
The 4th sound (S4)

Occurs just before S1. It is produced
by the augmented diastolic ventricular filling near the end of the diastole
and is caused by atrium contraction. It is loud due to a stiff ventricle.
It is a low-pitched sound and best heard with the bell of the stethoscope.
The ventricle can made stiff by : aortic stenosis, acute ischemia, hypertensive
heart disease and myocard infarct.
- S4 (Right ventricular) increased with inspiration.
- S4 (Left ventricular ) decreased with inspiration.
- Its is always abnormal.
- It indicates a lesser degree of ventricular dysfunction
than S3.
 S4.
S4.
Summation gallop

Occurs when both S3 and S4 are present
in a patient with tachycardia. Diastole may be shortened and the two sounds
may be merged.
 Summation
gallop.
Summation
gallop.
Ejection,systolic click

Heard in early systole and it represent,
aorta stenosis or systemic hypertension.
 Ejection
systolic click.
Ejection
systolic click.
Mid systolic click

Occur in mitral prolapse.
 Mid
systolic click.
Mid
systolic click.
Diastolic sounds
Opening snap.
Precedes the mid diastolic murmur
of mitral stenosis when not calcified. Rare is tricuspid stenosis. Often
heard at the apex or at the left sternal border. It is best heard with
the diaphragm of the stethoscope.
- Loud: Elastic valve leaflets.
- Soft: Sclerosis, calcification of the valve,
fibrosis.
 opening
snap.
opening
snap.
Murmurs
Murmurs may be systolic, diastolic,
or continuous. High-pitched are best heard with the diaphragm, low-pitched
with the bell of the stethoscope.
- Timing (systolic diastolic ).
- Intensity grade (see below ).
- Quality (crescendo- decrescendo).
- Location.
- Pitch.
- Changes by respiration, or position.
- Radiation.
Grade
Murmurs are graded according to
their intensity.
- Grade 1: barely audible with the utmost concentration.
- Grade 2: soft, but easily heard.
- Grade 3: loud without a thrill.
- Grade 4: loud with a thrill.
- Grade 5: loud with barely any contact between
stethoscope and chest.
- Grade 6: loud, heard with the stethoscope off
the chest.
Regurgitant murmurs:
Occur when a valve is meant to be
closed, and it is not.
Stenotic murmur:
Occur when a valve meant to be fully
open, and it is not.
Systolic murmurs

ejection murmur
this originate from the turbulent
flow through narrowed or irregular valves or outflow tracts. It has a crescendo-
decrescendo, diamond-shaped character.
- Normal: In children and infants, a soft systolic
murmurs may occur without significance.
- It is also common in a high output state (pregnancy
and tachycardia) .
- Aortic stenosis: Is best heard in the 2nd intercostal
space at the right of the sternum. It radiates to the neck.
- Pulmonic stenosis: Is best heard to the left
of the sternum in the 2nd intercostal space en does not radiate widely.
- Hypertrophic obstructive cardiomyopathy: Best
heard at the lower left sternal border. It increases with Valsalva strain
(raised thoracic pressure which impedes venous return ) and standing. It
does not radiate to the neck.
- Mitral valve insufficiency: With the patient
leis on the left lateral decubitus position. Best heard at the apex of
the heart. It radiates toward the left axilla and varies with intensity.
- Tricuspid regurgitation: Best heard at the lower
left sternal edge over the xiphoid. It increases with ventricular filling
(inspiration ). It is a softer murmur than mitral regurgitation.
 Aotra
stenosis,
Aotra
stenosis,  Mitral
insufficiency.
Mitral
insufficiency.
holosystolic murmur

A holosystolic murmur is do to regurgitation
or shunts into chambers that throughout systole are at lower resistance.
- Ventricular septal defect: Heard at the left
sternal edge in the 4th intercostal space. Louder with a increasing gradient
over the ventricul. Softer when decreasing the gradient such as with pulmonary
hypertension.
 Holosystolic.
Holosystolic.
Diastolic murmurs
Early diastolic murmurs :
Listen in the early diastole, for
the absence of silence.

- Aorta regurgitation: Blowing, high-pitched decrescendo
sound. Heard along the left sternal edge and toward the apex.
- Pulmonic regurgitation: High-pitched decrescendo.
Heard at the second left intercostal space at the sternal edge. It radiates
toward the mid-right sternal edge.
- Graham steel murmur: This is when pulmonary regurgitation
is secondary to pulmonary hypertension, which is itself due to mitral stenosis.
 Aorta
regurgitation.
Aorta
regurgitation.
Mid diastolic murmurs

- Mitral stenosis :Low-pitched apical diastolic
murmur.Best heard after mild exercise. The patient is in left lateral decubitus
position. The sound is best heard at the apex .
- Austin Flint murmur: Is due to fluttering of
the anterior mitral valve cusp, caused by the regurgitant stream from aorta
regurgitation.
- Carey Coombs murmur: Is due to thickening of
the mitral valve leaflets witch is caused by rheumatic fever.
- Tricuspid stenosis : Heard in 4th and 5th intercostal
space at the left sternum. It increase with: inspiration, sitting forward
and exercise.
 Mitral
stenosis.
Mitral
stenosis.
Continuous murmurs

Continuous murmurs indicate a constant
shunt flow throughout systole and diastole and may be due to patent ductus
arteriosus. It is loudest at the 2nd intercostal space just below the medial
end of the left clavicle.
- Coarctation of the aorta or pulmonary artery.
- Aorticopulmonary window murmurs : Are central
and at the 3rd intercostal space level.
- Branch stenosis of the pulmonary artery : Heard
more diffused through the chest.
- Systemic or pulmonic A-V fistulas: Heard also
more diffused through the chest.
- Congenital malformation.
- Coronary-cameral fistulas.
- Aorto-right ventricular or aorto-right atrial
fistulas: The communications are best heard directly over the lesions
 Dutus
arteriosis.
Dutus
arteriosis.
Pericardial Friction Rub

The sound has the character of pieces
of leather squeaking as they are rubbed together. Is a superficial, high-pitched,
or scratchy sound that may be systolic, diastolic or triphasic. The rubs
are best heard with the patient leaning forward or upon hands and knees
with breath held in expiration.
 Pericardial
rub.
Pericardial
rub.
Author: Jos-Paul Scholten
Last Revision: 01 Sept 1998
Coments e-mail:
 medicine@xs4all.nl
medicine@xs4all.nl















